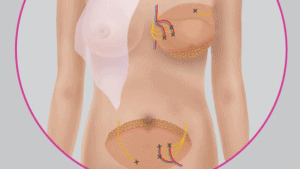
Rintarekonstruktiot
Rinnan rakentaminen rinnan poiston jälkeen auttaa rintasyöpäpotilasta toipumaan vakavasta sairaudestaan ja sopeutumaan takaisin normaalielämään.
Perinteinen rintasyövän hoito, jolloin yleensä rinta poistettiin ja kainalon imusolmukkeet tyhjennettiin, aiheutti naiselle paljon fyysisiä (esim. käden ongelmia, turvotusta, vartalon epäsymmetriaa) sekä sosiaalisia ja psyykkisiä ongelmia.
Tänä päivänä leikkausmenetelmien kehittyminen rintasyöpäkirurgiassa sekä mahdollisuudet rinnan rakentamiseen vähentävät näitä ongelmia ja tukevat potilaidemme laadukasta elämää vakavasta sairaudesta huolimatta.
Rintarekonstruktio rintasyöpäleikkauksen yhteydessä tai sen jälkeen
Rinta voidaan toisinaan rakentaa jo syöpäleikkauksen aikana tai sitten, kun potilas on toipunut rintasyöpähoidoista. Tähän menee aikaa yleensä pari vuotta. Korkean riskin taudissa suositellaan kolmea toipumisvuotta.
Omakudossiirteillä saadaan paras rinta. Implantit, kudosvenyttimet ja rasvan siirto ovat myöskin kehittyneet ja tarjoavat hyvän vaihtoehdon hoikalla asiakkaalla, kun omaa kudosta ei ole tarpeeksi siirrettäväksi.
Tunteva rinta
LTT Helena Puonti on kehittänyt ”Tuntevan Rinnan” menetelmän, jossa navan alapuolella olevasta vatsapoimusta rakennetaan rinta siten, että myös kudosten hermot yhdistetään ja uudessa rinnassa voi olla normaali tunto. Tämä on ainutlaatuista maailmassa. Clinic Helena tarjoaa tätä menetelmää kaikille siihen sopiville rintasyöpäpotilaille.
Lue lisää Tuntevasta rinnasta täältä.